Template File: /www/wp-content/themes/stn2017/index.php | Template Hierarchy
WP version: 6.5.5
PHP version 8.2.21
The West of Scotland Paediatric team recently held their first Paediatric Major Trauma Study Day at the Major Trauma Centre in Glasgow.
The aim was to increase knowledge of the Scottish Trauma Network, and the services available at a Major Trauma Centre. Topics covered at the event ranged from Paediatric pelvic injuries and trauma imaging to outcome measures for brain injuries. Speakers included prehospital staff, consultant specialist surgeons and AHP staff to represent how Paediatric patients are treated and managed within a Major Trauma Centre from the front door, though their rehabilitation and discharge.
The event was available to staff both in person and online via Microsoft Teams, which proved popular with over 170 people attending the event. The importance of optional virtual attendance was highlighted with 70% of staff attending virtually. The event had attendees from across the West of Scotland Trauma, as well as staff from across Scotland, England, Wales and Northern Ireland.
Feedback received from attendees was extremely positive, with an average overall rating of 9 out of 10. Attendees praised the variety of the content and range of speakers across the entire Multi-Disciplinary Team within the trauma setting, as well as the remarkably patient story.
“Hearing the patient story and the recognition of the work of the Rehab team and MT Coordinators”
“Loved all of the different speakers and realising that it really is a multidisciplinary team effort and not just one individual”
The day proved so popular that the Team have planned to make this an annual event. They would like to once again thank all attendees, speakers and those who helped to support the day.
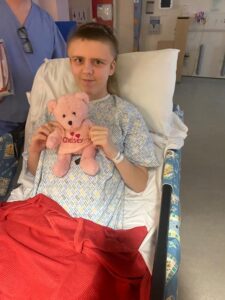
Chelsey Smith was 15 when she was left with life-threatening injuries, following a road traffic accident in February last year.
After an initial assessment at the University Hospital in Wishaw, Lanarkshire, Chelsey was rushed to the West of Scotland’s Paediatric Major Trauma Centre in Glasgow for specialist treatment.
Consultant Paediatric Neurosurgeon Roddy O’Kane performed the surgery, to reduce the swelling and pressure on Chelsey’s brain, with part of her skull being removed and stored in her stomach to keep it sterile.
Following intensive rehab with the team at the RHC, Chelsey, who is now 16, has made a remarkable recovery and, less than a year after her final surgery, was a guest of honour at the Major Trauma Centre’s training day this week.
She said: “I just can’t thank all of the team here at the Royal Hospital for Children in Glasgow for everything they have done for me, they have saved my life and given me my life back too.
“I don’t remember much about the day of the accident to be honest, but I’m here now and that’s what matters. I have had so much support from Roddy, my Major Trauma Co-ordinator Lynsay Stewart, all of the staff at the hospital and of course my family.
“Roddy was able to magically take a part of my skull and put it in my stomach to let the swelling reduce in my brain, I don’t really know how it works but it’s amazing. It was a long journey and I would tell anyone who is in a similar situation to keep going, to make this recovery you have to be mentally prepared for it too and thankfully I had so many positive people around me to help with that.”
Chelsey is now back preparing for her exams at Brannock High in Newarthill, has been able to get a part-time job and is hoping to go on to study accountancy.
She said: “Obviously everything that happened was not good, but thanks to the Royal Hospital for Children team in Glasgow I have been able to get back to school and have also started a part-time job.
“I just want to say thank you again to everyone for all they have done for me. Even after my follow-up appointments are finished, I’ll keep coming back to visit, I have missed them all.”
The procedure which involves removing part of the skull is not common, but after other medical interventions were unsuccessful it was the last option to save Chelsey’s life.
Roddy said: “This procedure is not something that we do every day but it gave Chelsey the best chance of surviving the injuries she had sustained during the accident.
“We take part of the skull out and store it in the stomach in order to keep it sterile, this is usually re-attached after a couple of months once swelling has reduced.
“Chelsey’s recovery is absolutely remarkable, based on her condition when she arrived it is incredible to see how well she is doing. There was a real danger to her life and we also anticipated that there would be more of lasting impact on her life.
“We are all so proud of Chelsey and all of the hard work she has put in during her rehab with our specialist teams. We’re delighted for her and her family and were all beaming from ear to ear when we got to see her again today.”
Paediatric trauma pathways in the NoSTN have been rolled out and developed since August 2019 across Grampian and Highland.
Over this time, service improvement projects have been carried out to improve delivery of care to these patients. Of significance are the number of patients to benefit from the trauma pathway within RACH who do not meet STAG inclusion criteria. The trauma pathway, which includes psychology and trauma coordinator input alongside relevant specialties and therapies, has allowed for a greater cohort of patients to access enhanced care following a traumatic injury. Services have also been extended to include burns patients where appropriate. We continue to promote our service and pathway by regular face to face promotion and posters throughout RACH to ensure familiarity and an easy referral process for staff.
Data collected for RACH between August 2019 and June 2022 shows that 89 patients have been commenced on the trauma pathway. Of those, 22 patients did not meet STAG inclusion criteria. This equates to roughly 25% of all patients. Comparison of both patient groups shows similar mechanisms of injury and patient/family needs following injury, further justifying the need for inclusion of patients out with audit criteria. Data shows that accidents involving motor vehicles and falls from height were the most common cause of traumatic injury. Numbers are also currently being collected to identify how many patients required psychology input following traumatic injury, with or without a rehab need. The intention has always been to improve patient care for all patient groups by creating a robust pathway which can be replicated. These figures highlight the far reaching benefits of this pathway, showing that clinical reasoning for individual cases ensures the most appropriate patients are encompassed.
Patient experience questionnaires have been developed for paediatric patients and their families. There are 3 different questionnaires aimed at 7-11 year olds, 12+ years and parents/carers. These are designed to gain positive feedback regarding service delivery as well as to identify areas of improvement. Comments received from recently completed questionnaires are below:

The paediatric trauma coordinator role recently adapted to include cross working over paediatric and adults MTCs. There have been many advantages to this. When an adult is admitted to hospital, their children’s lives are significantly disrupted. The child may not directly be involved in the trauma themselves. However, the dual role enables additional areas of support to be highlighted and provided for these families. Following education for adult colleagues, there is an increased awareness of child protection concerns. Links with paediatric services are now stronger and more efficient. There are times when a child/children and adult/s from the same family are admitted simultaneously. Having links with both hospitals enables smooth communication and visiting, joined up care and a consistent point of contact for the family. There is also a group of young people who may fall under adult services but whose needs very much lie within paediatric services. This can be dependent on age and stage, whether they are still a dependent living at home and whether they still attend school. Strong links with both teams ensures these patients have access to the appropriate professionals and that links can be made with schools/nurseries, families and third parties to ensure tailored support.
CBIT in Hand
We have recently established excellent links with our colleagues at the Child Brain Injury Trust. As a result, we have joined forces and launched the CBIT in hand app in RACH. This app is designed to provide information and advice following head injury to patients and families, professionals and third parties who come into contact with the child. Head injury may range from mild concussion through to traumatic brain injury. The app has been well received throughout the hospital by staff and patients alike. Details are being collected of those signposted to the app in order to gain feedback.
RACH Website
During the 2020 Covid pandemic, patients were contacted to gain information on preferred communication methods and access to information/resources. The responses overwhelmingly pointed to the need for online, electronic and easily accessible information. This was true from both patient and parent perspectives. It was identified that a platform for sharing such information was missing. Following research and networking around the hospital, it was found that this was a widely supported idea. Fast forward a few years and we are in the midst of RACH website development, having been lucky enough to secure the support and funding from the Archie Foundation. Once complete, this will feature a section for the Major Trauma Centre, helping to promote the identity of our service and provide easy access to online information for families.
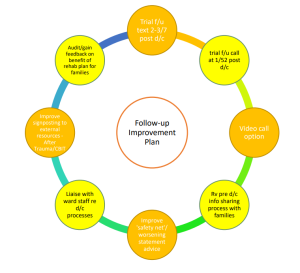
Follow-up Phone Call Audit
Patients who are commenced on the RACH trauma pathway will receive a follow-up phone call from the trauma coordinator after discharge. The purpose of the call is to provide safety netting, advice and action any outstanding issues which the family may have. An audit was completed to identify potential improvements to the follow up process for paediatric patients. Findings were as follows:

In October 2021 a team from RACH travelled to Orkney to undertake 2 days of paediatric trauma training. This involved lecture based education, multidisciplinary team simulation training with in situ practical procedures as well as question and answer sessions. Topics covered included chest and abdominal trauma, traumatic brain injury as well as child protection concerns and child death. The team thoroughly enjoyed their time there and the feedback was good. A similar trip is planned for September 2022 to Caithness General Hospital.
During Covid, the inpatient responsibility for those with head injuries moved from ED staff to the paediatric general surgeons. To try and ensure consistency with who was being admitted from ED, a proforma was created in accordance with SIGN guidelines. This has meant that decision making about who receives scans, who is observed, who is admitted etc is more streamlined and has led to clearer communication between the ED team and general surgery staff who look after these patients on the ward. The document has now been in circulation for over a year and we are looking at auditing its compliance in the near future. The remote and rural sites across the North of Scotland have also adopted this document. A similar inpatient proforma is also in circulation.
TRiM (Trauma Risk Management) is a trauma-focused peer support system developed to provide early help and information to staff who have experienced a traumatic/adverse/distressing event. Staff working in major trauma settings can be affected by a single distressing event or an accumulation of difficult/challenging situations. Indeed, this is relevant to working in a hospital setting more broadly and certainly not limited to major trauma. Enhanced staff support structures have been developed within RACH (and across NHSG) over the last few years. TRiM is one such development with an established pathway to request TRiM input following adverse events. Funding provided by the NoS Trauma Network enabled the Clinical Psychologist within the MTC pathway to complete TRiM training (practitioner and TRiM manager training) and contribute to the TRiM support available across RACH.
Written by Nina Currie (Paediatric Trauma Coordinator), Ashley Allan (Clinical Psychologist), Gillian Winter (Paediatric MTC Lead NoS/Specialty Doctor
Introduction by National Clinical Lead
Annual report time arrives once again, and in this new style of presentation my superlatives for the work of all who support the continued work, development and improvements of the Scottish Trauma Network will be brief. This is just as well, as the resources of my thesaurus begin to abate.
It is now 5 years since we convened and commenced our program of work to build and implement an entirely new clinical network of acute care and long-term rehabilitation for Scotland’s most seriously injured. August 30th 2021 witnessed the completion of Phase I with delivery of the fully operational end product. At time of writing, we run smoothly and successfully in the best traditions of “National Collaborative Pragmatism”.
All of this achieved of course, against the backdrop of complications presented to us by the pandemic. A remarkable achievement now recognised and acclaimed at the highest levels of the NHS, the Scottish Government, and national and international media.
This hard-earned and well-deserved reputation requires stiffening of the sinews and strengthening of resolve to be maintained, for us to progress further as we contribute well beyond our remit to the Remobilisation of the NHS in Scotland.
Thus, now begins Phase II, where we plan to tell the story using data, to raise standards for the future, and to demonstrate the sustained improved outcomes for patients, their families, their communities and the nation as a return on the visionary investment of these past 5 years.
The full report can be seen here
Martin McKechnie
National Clinical Lead
Scottish Trauma Network
The eighth report by the Scottish Trauma Audit Group (STAG) since 2011 can be found on the Public Health Scotland website. Compliance with a subset of the Scottish Trauma Network Key Performance Indicators, case-mix adjusted mortality and Patient Reported Outcome Measures (PROMs) are within part one of the report. Part two and three provide a comprehensive summary of injuries and the patient journey for both adults and paediatrics respectively.
Introduction from National Clinical Lead
2020 – 21 has been variously difficult, challenging, interesting and rewarding across the many spheres of activity, development and progress for the Scottish Trauma Network (STN). This Annual Report sits alongside and complements the imminent publication of the Scottish Trauma Audit Group’s (STAG) Annual Report for the same period. They both reveal and explore much of the data, operational and patient-centred clinical stories around this past year’s extraordinary activity within the Network. Set against the pandemic backdrop, the strong message coming from these reports is one of resilience, maintained high-quality patient care and an above-and-beyond spirit of collaboration and pragmatism on a national scale. That key performance and outcome measures have been delivered, yet alone maintained and improved in several areas, is worthy of acknowledgment and appreciation. The reports further explore much of our presentation and discussion at the Scottish Parliament Health and Sport Select Committee in January 2021.
There are many examples to celebrate, but I take this opportunity to highlight and express admiration and gratitude to the Scottish Ambulance Service, the ScotSTAR and EMRS transport and retrieval arms, and the newer Advanced Paramedics in Critical Care red teams therein. Their relentless and complex work in supporting and enabling the pandemic response across trauma and all related critical care services has been inspiring. The STN and patients are thankful to them beyond words. These thanks are expressed in equal measure to all staff and services recruited in good faith and optimism to the STN, yet who found themselves redeployed and reallocated to support the response in other vital areas such as Emergency Departments, Trauma Wards which became Covid High Dependency Units and Critical Care areas, and Theatres.
More interesting still is what much of this tells us about the improved access we now have to data and patient-reported measures. These are the mainstays of why the STN does what it does. With STN Trauma and STAG coordinators now embedded in our hospitals, we are able to reach more broadly across and deeper into the care of trauma patients than ever before. The resulting information and its analysis will further “tell the story” as we move beyond delivery of Phase I later this year, with the opening of the Major Trauma Centres at the Queen Elizabeth University Hospital in Glasgow, and the Royal Infirmary of Edinburgh, and the operational delivery of the Regional Networks in the West and South East of Scotland. These final pieces of the jigsaw will complete the national picture alongside the MTCs at Aberdeen Royal Infirmary and Ninewells Hospital in Dundee opened in 2018, supporting all the component services within our Regional Networks.
It is to be hoped that by the time of next year’s report we will be able to reflect upon a time of challenge and change with a more secure feel for what the immediate and medium-term future holds for our service. This learning allows us to reenergise and reconvene with strength, determination and the confidence that comes from surmounting such a significant hurdle.
Every person and every collaborative and linked service involved, described and embraced within the following pages is deserving of the greatest of gratitude and recognition. We are indebted to you all.
The full report can be seen here.
Martin McKechnie
National Clinical Lead
Scottish Trauma Network
While there are fewer other activities to divert us and our children during this period, it’s great to see everyone getting out on their bikes. It’s such a great way to get out and about and good for our general health and wellbeing. Safety equipment, such as helmets, can be helpful to keep their heads safe in case of a tumble, especially for children who are a bit less stable on their bikes. Mark Lilley, one of the Major Trauma Co-ordinators in Glasgow put together this short video with some advice when we had some glorious weather during lockdown last Spring/Summer. Keep cycling!
Image credit: Creative Commons, Pressedienst Fahrrad